Understanding Why Good Sleep Matters for Your Kidneys
Many of us know that sleep is essential for overall health, but few realise its significant impact on kidney function. If you or a loved one has chronic kidney disease (CKD), paying attention to sleep habits could be just as significant as following dietary recommendations or medication schedules.
Recent research has revealed a two-way relationship between sleep and kidney health. Poor sleep can worsen kidney function, while kidney disease itself often disrupts sleep. This article explores this vital connection and offers practical advice for improving your sleep quality.
How Sleep Affects Your Kidneys
The Impact of Sleep Duration
How much you sleep each night may directly influence your kidney health. Multiple large-scale studies have found connections between sleep duration and kidney function:
- Too little sleep: Sleeping 5 hours or less per night has been linked to a 79% higher risk of rapid kidney function decline compared to sleeping 7-8 hours.
- Slightly short sleep: Even getting just 6 hours of sleep is associated with a 31% increased risk of faster kidney function decline.
- Long-term effects: People who consistently sleep too little show a faster annual decline in kidney function measurements. Those sleeping 5 hours or less experienced about 1.2 mL/min/1.73m² decline annually, compared to 0.8 mL/min/1.73m² in those sleeping 7-8 hours.
- Too much sleep: Interestingly, regularly sleeping more than 9 hours may also be problematic. Studies from Japan found that extended sleep (8 hours or more) was associated with higher mortality rates in people with CKD, particularly in those under 65 years old.
These findings suggest an optimal “sleep zone” of about 7-8 hours for kidney health.
Guo S, Yamagishi K, Kihara T, Muraki I, Tamakoshi A, Iso H. Sleep duration and risk of mortality from chronic kidney disease among Japanese adults. Sleep Health. 2025 Feb;11(1):91–7.
Sleep Quality Matters Too
It’s not just about how long you sleep but how well you sleep. Research shows that:
- Having trouble staying asleep increases CKD risk by 13%
- Difficulty falling asleep raises the risk by 14%
- Regular use of sleeping pills or sedatives is linked to a 14% higher CKD risk
- People with severe sleep disturbances face a 61% higher risk of developing kidney problems
Bo Y, Yeoh E kiong, Guo C, Zhang Z, Tam T, Chan TC, et al. Sleep and the Risk of Chronic Kidney Disease: A Cohort Study. J Clin Sleep Med. 2019 Mar 15;15(3):393–9.Knutson
KL, Lash J, Ricardo AC, Herdegen J, Thornton JD, Rahman M, et al. Habitual sleep and kidney function in chronic kidney disease: the Chronic Renal Insufficiency Cohort study. Journal of Sleep Research. 2017 Jun 23;27(2):283–91.
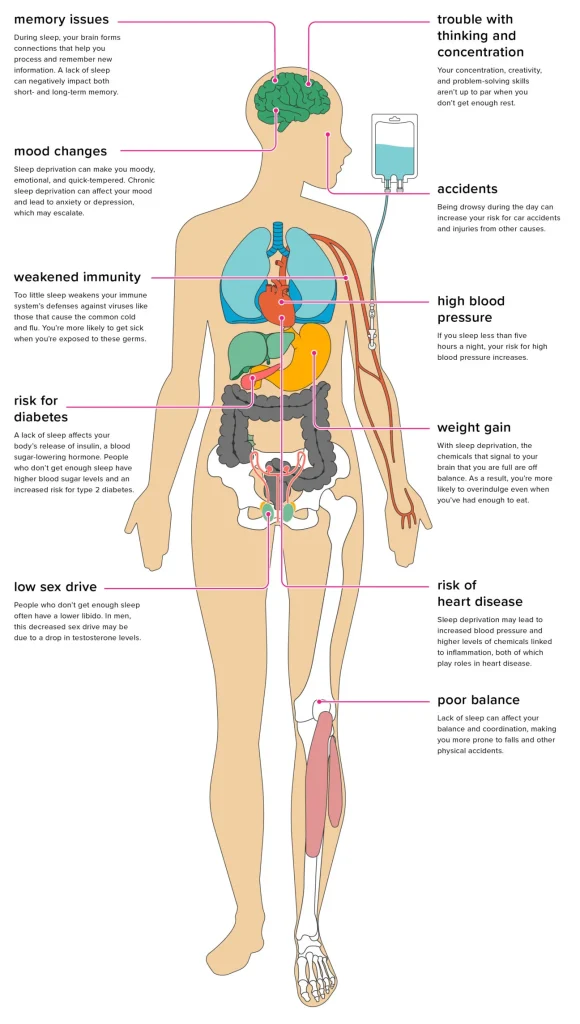
How Sleep Deprivation Harms Your Kidneys
When you don’t get enough quality sleep, several processes occur that can damage your kidneys:
Blood Pressure Effects
Poor sleep activates your sympathetic nervous system—the “fight or flight” response—which increases blood pressure. Typically, blood pressure decreases at night (“nocturnal dipping”), giving your kidneys a rest. Without this dip, your kidneys experience constant pressure, which can damage their delicate filtering structures over time.
Inadequate sleep disrupts your body’s ability to process glucose properly, creating insulin resistance similar to pre-diabetic conditions. Even if you don’t have diabetes, these changes can harm your kidneys in ways similar to diabetic kidney disease. Sleep deprivation also increases oxidative stress, essentially causing “rust” in your kidney cells and altering how your body processes fats.
Inflammation
Perhaps most concerning is that poor sleep triggers inflammation throughout your body. Studies show that sleep-deprived people have higher levels of inflammatory markers like interleukin-6, tumour necrosis factor-alpha, and C-reactive protein. This chronic inflammation directly damages kidney tissue and promotes scarring that can reduce kidney function over time.
How Kidney Disease Disrupts Sleep
People with CKD often experience sleep problems, creating a vicious cycle where kidney disease worsens sleep, which then further harms the kidneys. There are several reasons for this:
Uremic Toxins
When kidneys don’t function properly, waste products (uremic toxins) build up in the bloodstream. These toxins affect the brain regions that regulate sleep cycles and interfere with melatonin, your body’s natural sleep hormone. This makes it harder to fall asleep and stay asleep throughout the night.
Common Sleep Disorders in CKD
Several sleep disorders occur more frequently in people with kidney disease:
- Restless Legs Syndrome (RLS): Up to 40% of people with advanced CKD experience this condition, characterised by an irresistible urge to move the legs when resting. RLS can make falling asleep nearly impossible.
- Sleep Apnea: This condition, where breathing repeatedly stops and starts during sleep, is much more common in CKD patients. Fluid shifts, airway swelling, and changes in breathing control all contribute to its development in kidney disease.
- Periodic Limb Movements: These involuntary leg jerks during sleep fragment sleep patterns and contribute to daytime fatigue.
Calero K, Anderson WM. Can Poor Sleep Cause Kidney Disease? Another Step Closer to the Answer. Journal of Clinical Sleep Medicine. 2019 Mar 15;15(03):371–2.
Meng L, Ding Y, Li J, Li X, Yan T, Yang M, et al. Impact of inflammatory markers on the relationship between sleep quality and diabetic kidney disease. Sleep and Breathing. 2021 Apr 23;26(1):157–65.
Novak M, Winkelman JW, Unruh M. Restless Legs Syndrome in Patients With Chronic Kidney Disease. Seminars in Nephrology. 2015 Jul;35(4):347–58.
Practical Sleep Hygiene Tips for People with CKD
Improving sleep quality is a modifiable risk factor that could help protect your kidneys. Here are practical steps you can take:
Create a Sleep-Friendly Environment
- Control light exposure: Make your bedroom as dark as possible for sleeping. Use blackout curtains if necessary and remove electronics that emit light.
- Manage temperature: Keep your bedroom cool (around 65-68°F or 18-20°C) as this helps signal to your body it’s time to sleep.
- Reduce noise: Use earplugs, white noise machines, or fans to mask disruptive sounds.
- Invest in comfort: Ensure your mattress and pillows provide proper support. This is especially important if you have RLS or periodic limb movements.
Establish a Consistent Sleep Routine
- Set regular times: Go to bed and wake up at the same time every day, even on weekends. This helps regulate your body’s internal clock.
- Create a wind-down ritual: Develop a relaxing pre-sleep routine that might include reading, gentle stretching, or taking a warm bath.
- Limit bed activities: Use your bed only for sleep and intimacy to strengthen the mental association between your bed and sleep.
Manage Diet and Medication Timing
- Watch fluid intake: If you’re on fluid restrictions, plan your intake carefully to avoid excessive nighttime bathroom trips. Concentrate more fluids earlier in the day.
- Time your medications: Discuss with your doctor the best timing for diuretics and other medications that might affect sleep.
- Limit stimulants: Avoid caffeine after noon and nicotine close to bedtime, as both can interfere with falling asleep.
- Be cautious with alcohol: While alcohol might help you fall asleep initially, it disrupts sleep quality and can worsen sleep apnea.
- For Restless Legs Syndrome: Gentle stretching before bed, warm baths, and massage may help. Your doctor might check your iron levels, as iron deficiency can worsen RLS.
- For Sleep Apnea: If prescribed a CPAP machine, use it consistently. Sleeping with your head slightly elevated can also help reduce symptoms.
- For nighttime cramping: Gentle stretching and ensuring proper dialysis adequacy if you’re on dialysis may help reduce muscle cramps that disrupt sleep.
Mind-Body Approaches
- Practice relaxation techniques: Progressive muscle relaxation, deep breathing exercises, or meditation can help prepare your body and mind for sleep.
- Try cognitive behavioural therapy for insomnia (CBT-I): This proven technique helps identify and change thoughts and behaviours that cause sleep problems.
- Consider light therapy: Exposure to bright light in the morning helps regulate your circadian rhythm, especially if you have difficulty waking up.
When to Seek Professional Help
Speak with your healthcare provider if:
- You consistently have trouble falling or staying asleep
- You experience excessive daytime sleepiness despite adequate time in bed
- You have symptoms of sleep apnea, like loud snoring, gasping during sleep, or morning headaches
- Your bed partner notices unusual movements or behaviours during your sleep
- You have persistent symptoms of RLS that interfere with falling asleep
Integrating Sleep Care into Your Kidney Management Plan
If you have CKD, consider sleep as an essential part of your treatment plan:
- Mention sleep problems to your nephrologist or primary care provider
- Keep a sleep diary for two weeks before appointments to provide accurate information
- Follow through with recommended sleep evaluations, which might include overnight sleep studies
- Coordinate care between your kidney specialist and sleep medicine provider
- Reassess regularly, as sleep needs and problems may change as kidney disease progresses
Special Considerations
For Dialysis Patients
- Timing matters: Schedule dialysis sessions to avoid disrupting your regular sleep schedule.
- Address post-dialysis fatigue: Short naps (20-30 minutes) may help, but avoid long daytime sleep that could interfere with nighttime sleep
- Monitor for sleep apnea: Report symptoms promptly, as untreated sleep apnea is associated with worse outcomes in dialysis patients.
For Transplant Recipients
- Be aware of medication effects: Some anti-rejection medications can affect sleep quality.
- Monitor for new sleep disorders: Even after a transplant, sleep disorders may persist or develop.p
The connection between sleep and kidney health represents an essential but often overlooked aspect of CKD management. Both too little and too much sleep appear to affect kidney function, with quality of sleep playing an equally important role.
By improving your sleep habits, you’re not just enhancing your quality of life—you may also be helping to protect your kidney function. Small, consistent changes to your sleep routine could yield significant benefits for your overall health and potentially slow the progression of kidney disease.
Remember that improving sleep is a modifiable risk factor within your control. Work with your healthcare team to address sleep concerns and prioritise quality sleep in your kidney health management plan.